Diabetes has existed for as long as we can remember, and probably one of the most unfortunate things is that there’s still no cure on the horizon. There’s really nothing great when it comes to this matter, given the fact that thousands of people die yearly because of this disease, and even if it’s one of the oldest diseases ever, there’s still no cure for it.
But, in such cases, we can only try to look for the silver lining. In this case, it’s the fact that medicine has found ways to manage diabetes symptoms, and evolving technologies present new medical devices that help us live with it.
According to research conducted by the University of Manchester, it has been discovered that, in the UK alone, there are increasingly fewer people with type-2 diabetes getting HbA1c tests, which is the number one way to get information about your blood sugar levels over the long term. Hence, one ambition in the medical device and healthcare sectors is to create an ecosystem through technology, allowing patients to manage their illnesses more easily and get the right input from physicians remotely.
Ultimately, it would mean less money and wasted time on the patient’s behalf. In the latest Forbes article, one expert thoroughly explained how some medical technologists decided to offer a closed-loop system where the insulin pump receives information from a continuous glucose monitor to determine the needed insulin dose that should be administered accurately.
However, this level of caution is usually reserved for some of the most severe cases of type 1 diabetes. For other people with a more manageable variant, these devices might help:
Ketone monitor
For those who are suffering from diabetes, ketones, which are chemicals made in the liver and used for energy instead of carbs, might indicate if the condition is being controlled in an effective fashion by insulin provisions or not. This is mainly due to the fact that insulin allows the body to convert glucose into energy.
In some of the most serious cases, overproduction of ketones could make the blood a bit acidic, which is known as diabetic ketoacidosis. This kind of complication could ultimately lead to a diabetic coma and death. Even if this serious scenario is rare, especially for type-2 diabetes, devices that monitor ketones are on the market as an option for all sufferers who want to keep track of their ketone production but also gain a better understanding of how they should manage their condition. You’ve all heard of the ketogenic diet, a rather popular fitness trend.
Well, this diet spawned a breathalyzer ketone test. However, products made to detect chemicals in blood and urine have better accuracy, making them a better option when it comes to managing diabetes. It’s also worth mentioning that the breathalyzer is completely inaccurate once the user consumes alcohol.
Blood glucose monitor
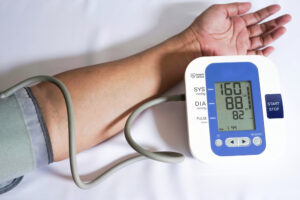
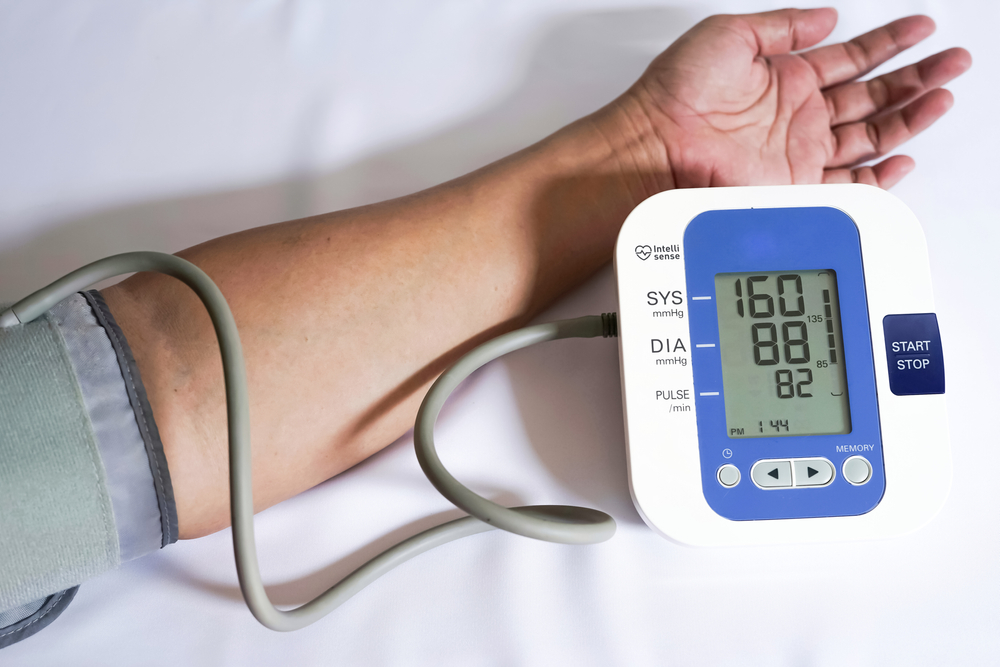
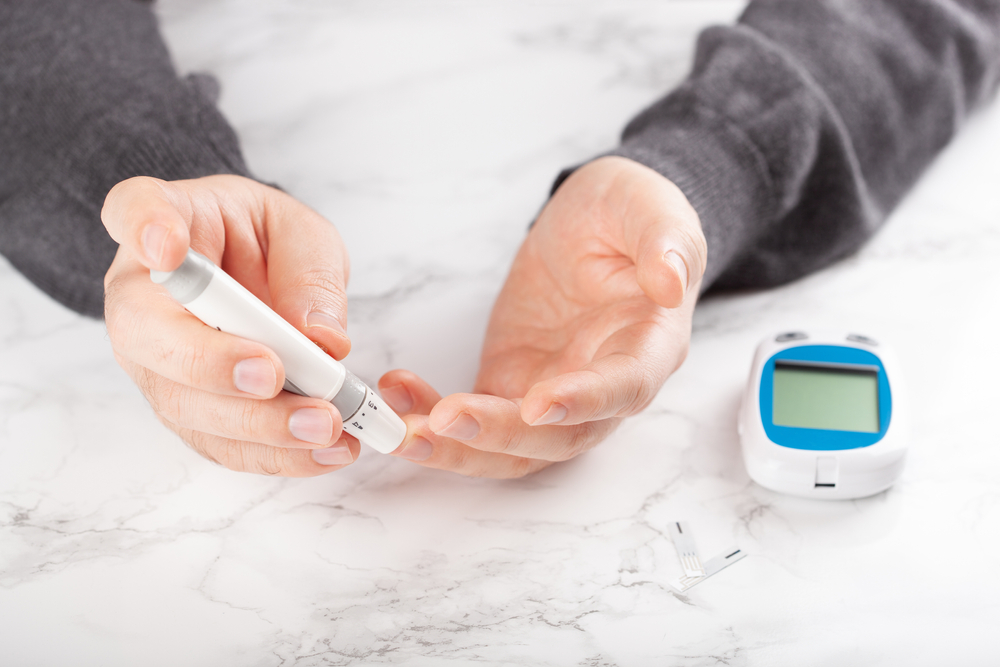
The first and most important measure of health for any patient with diabetes is their blood glucose level. As doctors measure the average blood sugar level over a period of 6 to 12 weeks using an HbA1c test, patients are also highly encouraged to use a blood glucose monitor between visits.
These devices usually require a blood sample, generally obtained through an included fingerprick implement, which will give an immediate glucose reading. This way, patients can know how well they manage their conditions at all times.
Remember that only a couple of glucose monitors on the market are so good; most of them can’t give a ketone reading, too. This monitor is way better for people who also want to manage their ketone levels.
Continuous glucose monitor
The continuous glucose monitor is seen by many as a natural evolution from the blood glucose monitor. It’s also easy to use: insert the sensor into a subcutaneous fat layer on your arms or stomach. Once you implant it, the sensor communicates with the transmitter that’s placed above it, which then communicates with a smartphone via Bluetooth in a timely fashion.
The transmitter triggers an alarm if the blood glucose levels are too low or too high. Don’t worry: the app will give you plenty of insight on how to deal with your glucose levels and what you can do to increase or decrease them as needed.
One of the best things about monitoring glucose is that you can share the data collected in the app with a physician. You can discuss this data and give them the proper insights into where the peaks and troughs might occur, which would eventually lead to better treatment and lifestyle advice.

Insulin pumps
When it comes to type one diabetes, which is the most severe of the two main types, the issue isn’t resisting insulin but the fact that the body can’t produce it in your pancreas as it should. Basically, patients with the disease are forced to inject themselves several times a day, and such a laborious process can be easily fixed with a pump. An insulin pump is an electronic device connected to a cannula inserted in the body near the waist, generally in the stomach area.
The pump can be easily set up to deliver doses of short-acting insulin, similar to how our pancreas functions. The device operates on a closed-loop system to which you can link a pump. It is built this way to automatically regulate and deploy the right dosage depending on real-time glucose levels.
Smart insulin pens
Some people might suffer from type 1 diabetes, so a pump could represent a viable option to replace insulin pens. You probably didn’t know this, but the standard method of insulin delivery before any other electronic device was ever made was the good old-fashioned pump.
However, for patients with type 2 diabetes, who rarely qualify for a pump in national healthcare and insurance-based systems, they only have a pen. Nowadays, insulin pens look slightly different from what they used to look like a decade ago. Now, they have built-in wireless communication systems and sensors, which allow patients to figure out the right amount of insulin delivery.
The pumps are also upgraded, as you have to connect the insulin pen to an app on a user’s smartphone, which will instantly allow you to input the latest blood glucose reading and get the right amount of insulin right away.

Diabetes management apps
Patients with type 2 diabetes are known to be insulin-resistant. That’s why they need to reconsider their lifestyle and diet choices, especially if they want to manage their blood glucose levels correctly. Many smartphone applications appeared on the market in light of changing behavior and habits.
These apps are meant to assist the task, which patients could integrate to leverage as much data as possible from other devices. OneDrop is probably one of the best examples, given the fact that its subscription-based services, which also include a Bluetooth glucose monitor, combine diet and exercise in their tools and offer patients one-on-one access to medical experts if they ever need further assistance. In some of the most recent studies, another famous app, Health2Sync, explored the option of using Fitbit.
Fitbit is a wearable device that can be used within a software platform to help patients connect with their doctors. This way, the study discovered in what ways the patient-doctor relationship can lead to better management of type-2 diabetes.
Interested to read more about useful gadgets and apps? Here’s what we recommend: 9 Must-Have Appliances EVERY Senior Should Have at Home